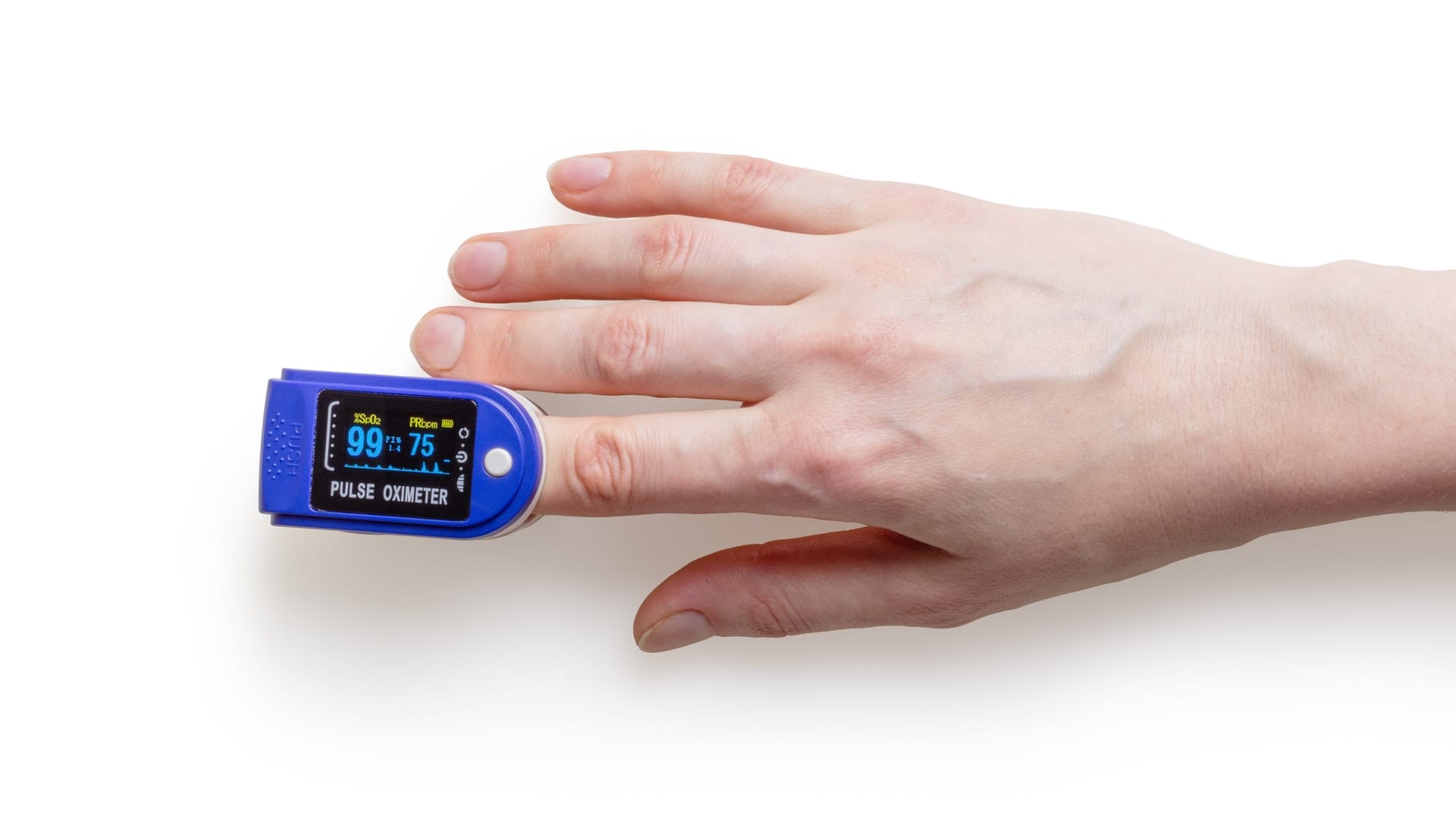
Pulse Oximetry is a technology used to measure the oxygen level in blood and heart rate and detect changes in the blood oxygen level.
Overview
Pulse oximetry has become the standard of care in operating rooms, intensive care units (ICUs), and hospital wards. Before pulse oximetry was available, physicians relied on invasive procedures, such as arterial puncture for blood gas analysis, to identify the presence of hypoxemia.
Definition of Pulse Oximetry
Hemoglobin can be functional or nonfunctional regarding oxygen binding and transport. Functional hemoglobin binds and transports oxygen and is present as oxyhemoglobin, which is hemoglobin containing bound oxygen, and deoxyhemoglobin, which is reduced hemoglobin, Without bound oxygen. Non Functional hemoglobin is unable to bind or transport oxygen and is present as carboxyhemoglobin and methemoglobin. Carboxyhemoglobin is hemoglobin bound to carbon monoxide. Methemoglobin is hemoglobin that contains ferric iron. The partial pressure of oxygen dissolved in arterial blood is termed, PaO2). The percent saturation of oxygen bound to hemoglobin in arterial blood is termed SP02.
Indication of Pulse Oximetry
Pulse oximetry is indicated in all clinical settings in which hypoxemia may occur, Such as operating rooms, ICUs, post-anesthesia care units, emergency departments, ambulances, endoscopy suites, sleep laboratories, cardiac catheterization laboratories, delivery suites, and Wards. Pulse oximetry can also be used to screen for cardiopulmonary disease. It is safe to use in monitoring all patients.
Principles of operation of Pulse Oximetry
Pulse oximeters consist of a peripheral probe and a microprocessor unit. Traditionally, the external probe contains a photodetector and two light-emitting diodes. The light emitted by the diodes is absorbed by tissues, and the amount of absorption is determined by the photodetector. It calculates the percentage of oxyhemoglobin and displays the hemoglobin oxygen saturation in arterial blood. Pulse oximeters function on the principle that oxygenated hemoglobin and deoxygenated hemoglobin absorb red and infrared light differently. One light-emitting diode emits light in the red spectrum, at a wavelength of 660 nm, at which the light absorption of deoxyhemoglobin is higher than that of oxyhemoglobin.
The other diode emits light in the infrared spectrum, at a wavelength of 940 nm, at which oxyhemoglobin absorbs more light than deoxyhemoglobin. The microprocessor analyzes the light absorption of the tissues at each wavelength to determine the concentrations of oxyhemoglobin and deoxyhemoglobin, respectively. The probe is positioned so that the photodetector and light-emitting diodes face each other.
During pulsatile flow, the light absorption of arterial blood, background tissues, and venous blood are detected. During non-pulsatile flow, only the light absorption of background tissues and venous blood is detected. The micro-processing unit compares the light absorption during both pulsatile and non-pulsatile flow to isolate the light absorption of arterial blood and determine the SpO2.
Best 5 Pulse Oximeter with Low Price 2021

Acc U Rate 430-DL Premium Fingertip Pulse Oximeter Oximetry Blood Oxygen Saturation Monitor with silicon cover, batteries, and lanyard by CMS

Innovo Premium Fingertip Pulse Oximeter Blood Oxygen Monitor with Plethysmograph and Perfusion Index
by Innovo

Santamedical Generation 2 OLED Fingertip Pulse Oximeter Oximetry Blood Oxygen Saturation Monitor with batteries and lanyard – Silver
by Santamedical

Active Health Labs Fingertip Pulse Oximeter – Blood Oxygen Saturation and Pulse Monitor
by Active Health Labs

Deluxe SM-110 Two Way Display Finger Pulse Oximeter with Carrying Case and Neck/Wrist Cord
by Santamedical
Data interpretation of Pulse Oximetry
Pulse oximetry provides both qualitative and quantitative data. The qualitative data are obtained through the sounds emitted by the pulse oximeter; these sounds correlate with oxygen saturation. The quantitative data are obtained by displaying a pulsatile Waveform that corresponds to the flow of arterial blood, and the display of numbers indicates the SPO2) and the heart rate.
Proper use of pulse oximetry
The ideal site for placement of the pulse oximeters probe is Well perfused, relatively immobile, comfortable for the patient, and easily accessible. If the probe is not the right size, the light-emitting diodes may not line up correctly with the photodetector and may produce inaccurate data.
Common problems and limitations
One common problem is the occurrence of movement artifacts if there is movement at the probe placement site. This may interfere with proper function and most often occurs if a patient is shivering or seizures. Electromagnetic radiation, such as that emitted by magnetic resonance imaging (MRI), may also interfere With pulse oximetry. If the probe is poorly placed or is the Wrong size, light from only one light-emitting diode may pass through tissues, or the light may not reach the detectors.
The presence of intravascular dyes, such as methylene blue or indigo carmine, may alter the red and infrared light absorption properties of tissues, leading to an inaccurate reading. Methemoglobin absorbs more light than either deoxyhemoglobin or oxidized hemoglobin at 940 nm, but at 660 nm, the light absorption of methemoglobin is similar to deoxyhemoglobin. In this instance, the pulse oximeter cannot differentiate between methemoglobin and deoxyhemoglobin and may incorrectly perceive an elevated deoxyhemoglobin concentration.
It is important to remember that pulse oximeters function normally in anemic patients with reduced numbers of red cells. In an extremely anemic patient, the oxygen saturation may be normal, but insufficient hemoglobin may carry an adequate amount of oxygen to the tissues.
A normal SpO2 may be falsely reassuring in patients receiving Supplemental oxygen because a drop in SPO2 may occur only after the patient is severely hypercarbia. New generation pulse oximeters are manufactured with improved algorithms that minimize motion-related erroneous data.
Besides, because they use multiple Wavelengths, these new pulse oximeters can measure the concentration of hemoglobin, carboxyhemoglobin, and methemoglobin.
Complications of Pulse Oximetry
Although the pulse oximeter is generally a safe device, its use still carries some adverse events. Burning or blistering at the placement site may occur if the light-emitting diode becomes overheated. Ischemic pressure necrosis may result if the probe is placed too tightly on the patient. Prolonged placement of a pulse oximeter probe, which can occur in the ICU, may lead to mechanical injuries, such as finger stiffness, making it difficult for the patient to flex the finger after the probe has been removed.
Summary
When used correctly, pulse oximetry is a potentially lifesaving tool. Health care providers need to be aware of the indications, benefits, and disadvantages of pulse oximetry. More important, clinicians must be able to interpret the information pulse oximetry provides. With proper training and instruction, clinicians Will find pulse oximetry an irreplaceable monitoring tool.
Reference: NEJM April 21, 2011: 364; 16